Pressure Therapy (Compression Garments and Clips)
Last reviewed: April 2026
Evidence rating reflects the quality and volume of research — not how well the treatment works. How I grade evidence →
Sustained mechanical pressure delivered to the scar through custom garments, silicone discs, or spring-loaded ear clips. One of the oldest evidence-based interventions in scar medicine — pressure therapy is a backbone treatment for burn-related hypertrophic scars and a standard adjunct for ear keloids after excision, where it consistently lowers recurrence compared with surgery alone.
How it works
Continuous external pressure (target range 15-40 mmHg depending on site) does several things at once: it reduces local blood flow and oxygen tension within the scar, which slows the fibroblast activity that drives collagen overproduction; it mechanically flattens and reshapes immature collagen bundles before they mature into the disorganized, thickened architecture typical of keloids; and it down-regulates TGF-β1 signalling and upregulates matrix metalloproteinases (MMPs) that break down excess scar tissue. The effect is dose-dependent on time — most evidence suggests pressure needs to be worn 18-23 hours per day to produce meaningful change, and less than around 15 mmHg sustained pressure is generally considered sub-therapeutic. This is why garment design, fit, and daily wear compliance matter far more than which brand of garment you use.
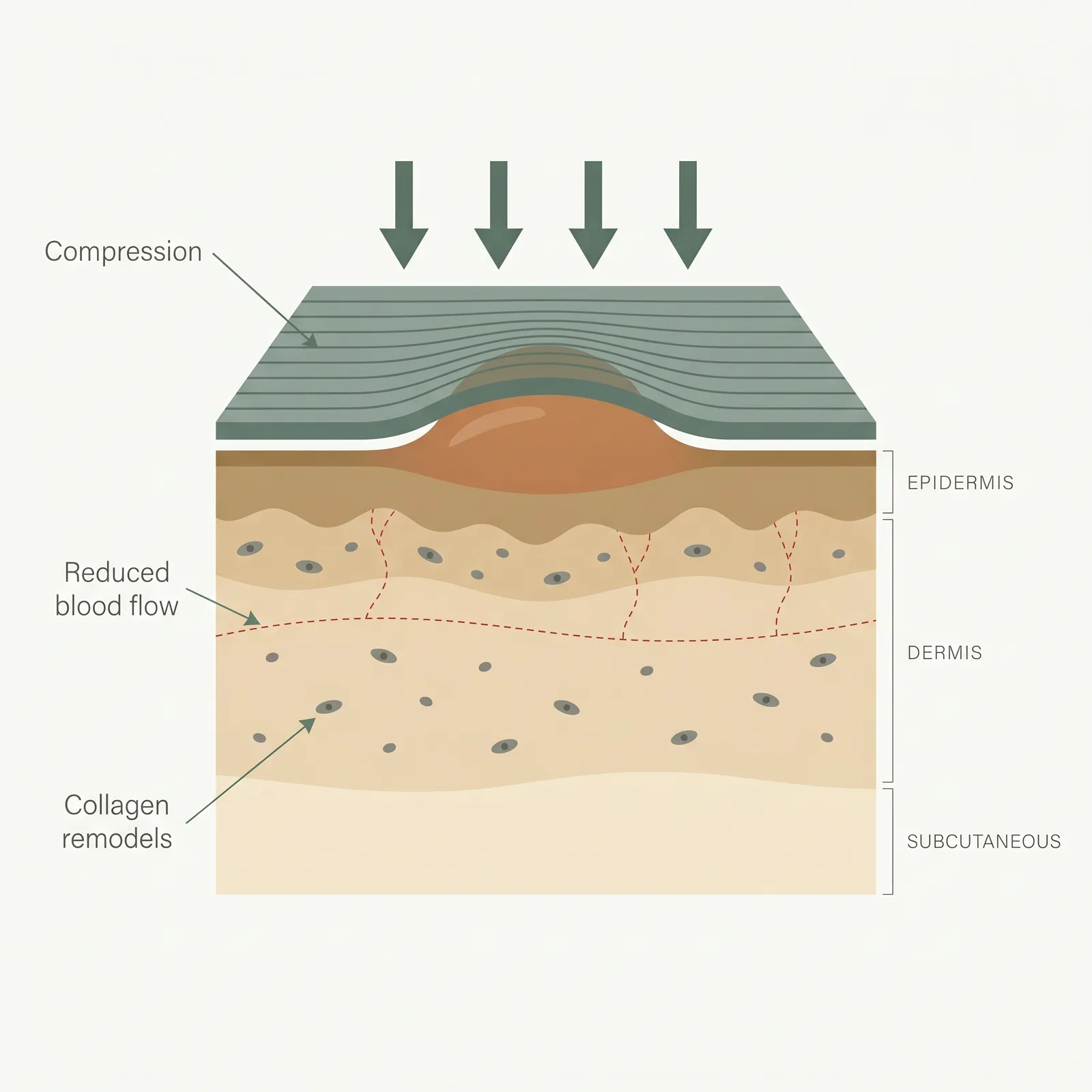
- 1Sustained pressure. Garments and clips apply 15–25 mmHg continuously for 18–23 hours per day over many months.
- 2Reduced perfusion. Pressure lowers local blood flow and oxygen tension inside the scar, calming its inflammatory drive.
- 3Collagen remodeling. With less fibroblast fuel, the scar gradually flattens and reorganizes — clearest on burn and ear keloids.
Typical protocol
Worn 18-23 hours per day for 6-12 months (up to 2 years for large burn scars). Ear keloid clips are typically worn 12-16 hours per day for 6-12 months post-excision, often alongside steroid injections. Custom-fitted garments are refitted every 2-3 months as the scar flattens and swelling reduces.
- Time to results
- Softening and reduced redness at 3-6 months; meaningful flattening and architectural remodelling over 12-24 months.
- Accessibility
- widely available
- Recurrence
- 15-30% for ear keloids when used consistently post-excision with steroid injection support
- Insurance
- sometimes
Best for
- • Post-surgical recurrence prevention, especially earlobe and ear cartilage keloids
- • Burn-related hypertrophic scarring (where pressure therapy is standard of care)
- • Young, immature scars in the first 6-12 months when collagen is still being laid down
- • People who prefer a non-injection, non-procedural option
- • Anatomically amenable sites (ears, limbs, torso) where a garment or clip can maintain contact
- • As a long-term maintenance layer alongside other protocols
Limitations to know
Combining with other treatments
Pressure therapy is almost always used alongside another modality. The strongest combination in keloid care is post-excision pressure plus intralesional triamcinolone for ear keloids — the combination consistently reports recurrence rates in the 15-30% range versus 45-100% for surgery alone. Pressure pairs naturally with silicone sheeting (many products combine both), with red-light therapy as a daily calming layer, and with post-burn physiotherapy protocols. For ear keloids specifically, a pressure clip is often worn during waking hours and a silicone sheet overnight to cover the full 24-hour window. Avoid applying high pressure over fresh wounds before full closure.
Evidence sources
Pressure Garment Therapy for Hypertrophic Scars
2009Anzarut A, Olson J, Singh P, et al. · Journal of Plastic, Reconstructive & Aesthetic Surgery
Meta-analysis showed pressure garment therapy produced small but statistically meaningful improvement in scar height, thickness, and global assessment scores for hypertrophic burn scars.
View source →Surgical Excision and Postoperative Compression for Ear Keloids
2012Park TH, Seo SW, Kim JK, Chang CH · Archives of Plastic Surgery
Excision plus continuous compression for 6-12 months substantially reduced recurrence of ear keloids compared with excision alone, with recurrence rates around 10-15% when compression was maintained.
View source →Mechanomodulation of the Scar Microenvironment: Evidence, Mechanisms, and Clinical Translation
2016Ogawa R, Akaishi S · Wound Repair and Regeneration
Mechanistic review showing that mechanical forces directly modulate keloid fibroblast behaviour through mechanotransduction pathways; pressure and tension management is now considered central to scar outcomes.
View source →Effectiveness of Silicone Gel Sheet and Pressure Therapy on Hypertrophic Scars: A Randomized Controlled Trial
2010Li-Tsang CW, Zheng YP, Lau JC · Journal of Burn Care & Research
Combined pressure + silicone therapy outperformed either modality alone on scar thickness, pigmentation, and pliability — foundational evidence for the layered protocols used in modern burn scar care.
View source →
Frequently asked questions
How much pressure is therapeutic, and how do I know I'm getting it?
The commonly cited therapeutic range is 15-25 mmHg for garments and 15-40 mmHg for ear clips, sustained continuously. Below about 15 mmHg, pressure is generally considered sub-therapeutic. In practice you won't feel a number — but you should feel firm, consistent contact that leaves a gentle temporary indent when removed. A garment or clip that slips, twists, or feels comfortable enough to forget about is usually under-pressured. Custom burn garments are built to pressure specifications; off-the-shelf ear clips often have adjustable spring tension so you can dial in a firm but tolerable level.
How many hours per day do I really need to wear it?
The burn-scar literature converges on 18-23 hours per day for hypertrophic scars and 12-16 hours for ear keloid clips. Taking it off only for bathing and short breaks is the standard recommendation. Compliance is the single strongest predictor of outcome — a correctly fitted garment worn 20 hours a day outperforms a better garment worn 10 hours. If a schedule that demanding isn't realistic, combine a daytime clip with an overnight silicone sheet to cover more of the 24-hour window with less friction.
How long until I can stop wearing it?
Most protocols run 6-12 months for ear keloids and 12-24 months for burn-scar garments, stopping once the scar has been stable and mature for several months. Stopping too early — while the scar is still pink, itchy, or actively remodelling — is a common cause of rebound thickening. Your dermatologist or burn therapist should reassess every 2-3 months and phase you off gradually rather than all at once. Some people transition to nighttime-only wear for another 3-6 months as a taper.
Does pressure therapy work on its own, or do I need to combine it?
It rarely works alone on an established keloid. Its strongest evidence is as a prevention tool (post-excision, post-burn) and as a combination layer alongside silicone, steroid injections, or both. For someone with a new ear keloid considering excision, the combination of surgery + steroid + pressure clip is one of the most reliable recurrence-reduction protocols in the literature. For an existing, untreated keloid, pressure can soften and calm it somewhat but is usually not enough to flatten it without adjunct therapy.
Can pressure therapy cause problems on its own?
Occasionally. Overly tight or poorly fitted garments can cause skin maceration, heat rash, itching, or, rarely, pressure ulcers on bony prominences. Children need especially careful monitoring because ill-fitting garments can affect growth and breathing if applied over the torso. For ear clips, excessive spring tension can cause cartilage pain or ischemia — firm should feel like pressure, not pinching. If you have ongoing pain, blanching that doesn't return, or skin breakdown under the garment, stop and see your provider to have it refitted.
Medical disclaimer
ScarInsight provides educational information about scar and keloid treatments based on published research. This content is not intended to diagnose, treat, or prevent any medical condition. Individual results vary. Treatment decisions should be made in consultation with a qualified dermatologist or healthcare provider who can evaluate your specific situation. ScarInsight is not a healthcare provider and does not offer medical advice.